1. Introduction
© W. Isaranuwatchai, R. A. Archer and A. J. Culyer, CC BY 4.0 https://doi.org/10.11647/OBP.0195.01
1.1 Non-Communicable Disease
Non-communicable diseases (NCDs) are the leading cause of death worldwide and contribute to over 73% of all deaths annually.1 Each day, NCDs cause more than 100,000 deaths; 80% of which occur in low- and middle-income countries (LMICs).2 Over the last 30 years, NCDs have replaced communicable diseases (CDs) as the cause of greatest health burden.3 This trend is evident in the risk factors for NCDs. According to the World Health Organization (WHO), obesity has tripled since 1975;4 while the International Diabetes Federation estimates that the global prevalence of diabetes, 8.8% in 2017, will increase by 48% by 2045, with an additional 204 million people living with diabetes.5 Much of this burden could be completely avoided because NCDs are largely preventable.6 Approximately 40% of all cancers and three-quarters of the incidence of heart disease, stroke and type 2 diabetes could be prevented by addressing tobacco use, unhealthy diet, physical inactivity and harmful use of alcohol. A great deal of technical knowledge exists about how to prevent and manage NCDs, such as the WHO Package of Essential NCD interventions (WHO PEN),7 the SHAKE8 (the technical package for salt reduction) and HEARTS9 (the technical package for cardiovascular disease management in primary health care) packages.
In addition to the NCD burden,10 there is an increasing demand on governments to address the health needs arising from NCDs through universal health coverage (UHC) policies, a direction that has been endorsed by the World Health Assembly11 and the United Nations General Assembly.12 NCDs are the result of various factors, for example genetic, physiological, and environmental and behavioral13 individually or in combination. They frequently require a collective response. They are not contagious, unlike communicable or infectious diseases, which can be spread, directly or indirectly, from one person to another.14 CDs, accidents and injuries also often need collective actions (such as mass vaccination or health and safety legislation) for effective treatment but can also be treated effectively on an individual basis. There are noticeable patterns in prevalence and mortality between CDs and NCDs. Figures 1.1 and 1.2 show the prevalence and mortality of CDs and NCDs in high-income countries (HICs), LMICs and around the globe.15 CDs are prevalent (~70%) in HICs compared to ~45% in LMICs (Fig. 1.1). NCDs are more prevalent in LMICs (~55%) compared to HICs (~30%). From the 37 years of data examined for Global Burden of Disease Study 2016, NCDs now dominate premature death.16 Over 80% of the world’s premature deaths are attributable to NCDs in LMICs.17 The probability of premature death from NCDs is almost four times higher in LMICs compared to HICs.18
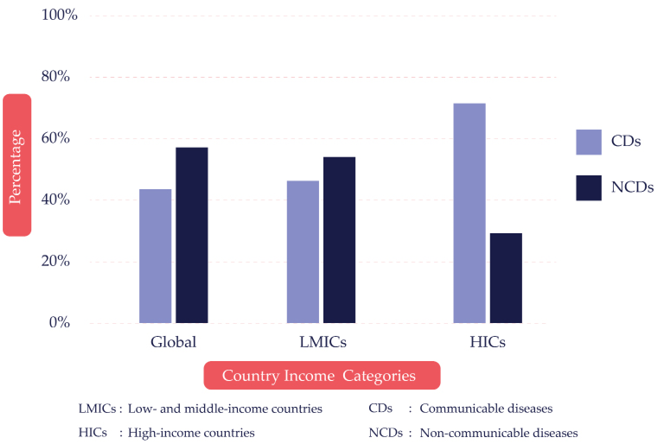
Fig. 1.1 Prevalence of CDs and NCDs by World Bank country income categories.19
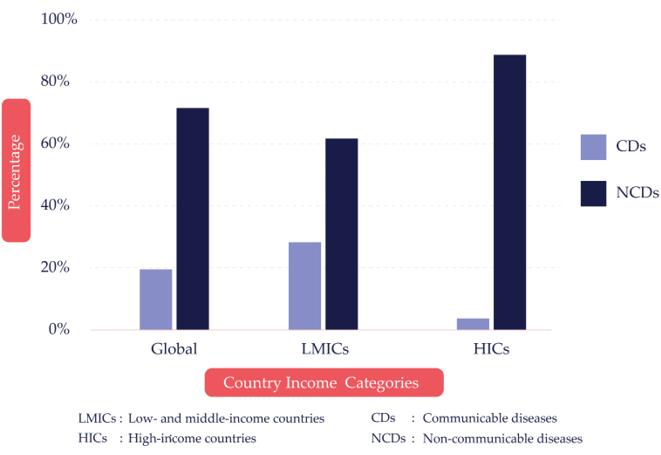
Fig. 1.2 Deaths from CDs and NCDs by World Bank country income categories.20
NCDs represent a significant burden through both an epidemiological and an economic lens.21 They affect everyone regardless of sex and age.22 The four main NCDs are cardiovascular disease, chronic respiratory disease, cancer and diabetes, which account for over 80% of NCDs deaths.23 A macroeconomic simulation model suggested a cumulative loss of USD $47 trillion over the next 2 decades due to NCDs.24 The Disease Control Priorities 3rd edition (DCP3) estimated that the number of deaths averted through prevention in LMICs could be between 2 to 4.2 million by 2030.25 Additionally, mental health problems are the leading cause of disability around the world.26 For example, approximately 800,000 people commit suicide every year and about 75% of those occur in LMICs.27 Mental health problems represent risk factors for other diseases such as cardiovascular diseases and diabetes including unintentional and intentional injury. There is significant inequity in the support (e.g., health services) for mental health around the world.
In an ideal world, it would be easy to prioritize interventions and allocate resources to have the maximum impact on health and its fair distribution, while simultaneously minimizing the risk to families of serious financial hardship from out-of-pocket payments. These are generally seen as the main concerns of cost-effectiveness analysis.Systems are, however, faced with a diversity of investment options, inescapable limits on resources, evidence that is at best sporadic, many other political, financial and social constraints, and a host of other additional28 considerations; all of which make identifying good value-for-money interventions challenging. The question naturally arises: why have we, the global community, not been more successful at reducing this NCD burden? Does a universal problem not have a universal solution? Is resource scarcity the fundamental culprit? Is cost-effectiveness really the answer? Are there better ways of using the resources that countries already have? Do countries have the essential human capital required to develop and roll out the right policies? Are there higher priorities for public spending against which the NCDs simply cannot compete? We try to answer these questions and make some suggestions for future actions in this book.
1.2 Best, Wasted and Contestable Buys
One response by the WHO to the NCD crisis was the idea of ‘Best Buys’. WHO defines Best Buys almost solely by their cost-effectiveness, that is, interventions which achieve best value for money in comparison to all comparators.29 More precisely, Best Buys for LMICs are interventions with an incremental cost-effectiveness ratio (ICER) under 100 International United States dollars per disability-adjusted life-year (DALY) averted.30
Some Wasted Buys are easy to define: they are interventions that have no beneficial effect. Others are slightly harder to specify, for they are interventions that do have a beneficial effect (with NCDs, the effect almost always lies in the more distant future) but ones that require too great a sacrifice of resources. That is, those resources would have a more beneficial effect used elsewhere on other health interventions or elsewhere in the economy. In other words, their opportunity cost is too high.
We suggest the addition of the category ‘Contestable Buys’ when there are suggestions that an intervention and its associated attributes may be a Best Buy but there is no direct evidence of cost-effectiveness in the local setting in which the intervention might be implemented. Thus, interventions in the WHO’s Best Buys list may be better classed as Contestable Buys if there is no demonstrative evidence of cost-effectiveness for the particular setting in question. The main distinction between Best and Contestable Buys is thus the availability of context-specific evidence.
1.3 Definitions and Central Ideas
Box 1.1 contains the definitions of central ideas that are used throughout the book. The reader will find these definitions to vary slightly from the many that lie elsewhere in the literature, though we are confident that any differences are minor and more questions of emphasis than of substance. We — all the authors here represented — have sought to be consistent in the way we have used these terms.
We refer frequently to ‘interventions’. This word is intended as an all-embracing term to capture a package of care over a relevant time period as applied to a particular condition or combination of morbidities. It may be restorative, maintenance or preventive. It may be provided in part from a health service program and partly from another like childcare or primary education. This is especially significant in the field of NCDs, with which this book is concerned. An intervention should not be seen as merely the purchase and use of a medicine, or any other single input, but rather as the planned or usual combination of human and physical resources required for the delivery of a service at a chosen standard. Some of these inputs may not be what we customarily think of as ‘healthcare’.
A critical starting point in determining the value of an intervention is its cost-effectiveness — if an analysis establishes empirical evidence of cost-effectiveness in the context of the location in which it is intended to be used, the intervention will be categorized as a ‘Best Buy’. If it establishes empirical evidence of its cost inefficiency, it will essentially be categorized as a ‘Wasted Buy’ or if it confers very little effectiveness, that is, the costs are not proportional to effectiveness, then it will again be categorized as a Wasted Buy.
Box 1.1 Definitions of Basic Terminology Used in Economic Evaluation
Economic evaluation is the comparative analysis of two or more alternatives in terms of their costs and outcomes. There are different types of economic evaluation, namely cost-benefit analysis, cost-minimization analysis, cost-utility analysis and cost-effectiveness analysis. They differ primarily in the measurement of consequences or outcome; however, each approach entails value judgements that should be explicitly considered in terms of their appropriateness in the decision context.
Cost-effectiveness analysis (CEA) is a form of economic evaluation that uses monetary units to measure/value costs and (usually) a single effect of interest that is common to the alternatives in consideration. The effect is measured in terms of clinical natural units (e.g., life-years gained). Often, cost-effectiveness analyses are interchangeable with cost-utility analysis that uses generic outcome measures such as the quality-adjusted life-year (QALY) or disability-adjusted life- year (DALY) instead of clinical natural effects. The advantage of the cost-utility analysis approach over cost-effectiveness analysis is that the former allows comparison of value in health investment between different health problems such as diabetes and mental health.
Disability-adjusted life-year (DALY) is a measure of overall disease burden, expressed as the total number of years of life lost due to ill-health, disability, or premature death. One DALY is equal to one year of healthy life lost.
Quality-adjusted life-year (QALY) is a measure of the state of health of a person or group, which is a function of the length and quality of life. One QALY is equal to one year of life in perfect health.
Incremental cost-effectiveness ratio (ICER) is calculated as the difference in cost between two possible interventions, divided by the difference in their outcomes. It is a standard measure representing marginal cost per marginal benefit from health investment.
Health Technology Assessment (HTA) is a form of evaluation that includes CEA but goes beyond its categories by including non-financial constraints and local environmental, organizational, social and political factors that may affect the costliness, effectiveness and feasibility of interventions.
Sources: adapted from Drummond et al., 2015 and Briggs et al., 2006.31
1.4 The Cost-Effectiveness Plane
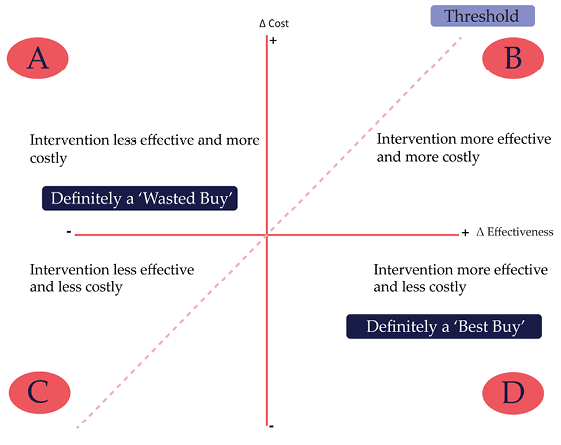
Fig. 1.3 Cost-effectiveness plane.
These ideas are illustrated by what is called a Cost-Effectiveness Plane. In Fig. 1.3, the health effects of an intervention are measured in terms of lives saved, QALYs, DALYs averted, or other suitable indicators on the horizontal axis (positive effects to the right and negative ones to the left). Its relative costliness is shown by the vertical axis. A comparator intervention can be understood to be at the origin where the two axes cross, so the health gain and the cost are both relative to a comparator. The distances along the axes measure the difference between the intervention under investigation and the comparator. The slope of the dashed line labelled ‘threshold’ indicates the willingness of the payer (usually an insurer or the government) to pay for additional health (ΔC/ΔE): the ICER. This threshold is also known as the cost-effectiveness threshold or willingness-to-pay (WTP) threshold and is expected to be different for each country setting.32 That being so, what is regarded as cost-effective will also differ according to country.
The area lying in quadrant D clearly identifies a Best Buy — the intervention is both more effective and less costly than a relevant comparator. The area lying in quadrant A is clearly a Wasted Buy. D and A are areas in which an intervention dominates or is dominated by the comparator in terms of cost-effectiveness and its position relative to the threshold. This analysis is a development of the approach taken by the Institute of Medicine’s (IOM) famous book Crossing the Quality Chasm.33 In discussing efficiency as one of the six specific aims for improvement in health care, the book asserts that ‘the opposite of efficiency is waste, the use of resources without benefit to the patients a system is intended to help’.34
What of areas B and C? An intervention falling in B could be either a Best Buy or a Wasted Buy. In quadrant B, the intervention is more expensive but it is also more effective, so the question become whether the additional effectiveness is ‘worth’ the additional expense. Here, the dashed line comes into play because cost-effectiveness will depend on the maximum amount the payer is willing to spend for additional health outcomes. When the intervention is located above the dashed line, the additional or incremental cost (ΔC) exceeds the payer’s willingness to pay for the additional or incremental health (ΔE), and the intervention will be judged to be cost-ineffective by the payer and therefore a Wasted Buy. Conversely, an intervention falling below the threshold line will be deemed cost-effective and therefore a Best Buy.
Quadrant C brings up some counter-intuitive possibilities. In this quadrant, the intervention is definitely less effective than the comparator. However, it is also less costly. Again, whether it would be a Wasted Buy depends on whether the cost savings of using it sufficiently compensate for using this intervention rather than its more effective comparator. How can this be? Only if the cost savings, if realized, can be used to generate more health elsewhere. In quadrant B, the threshold line indicates the maximum willingness of the payer to pay for additional units of health. In quadrant C, the line indicates the minimum the payer is willing to accept to forgo a marginal health benefit. If the threshold genuinely indicates the payer’s judgment of value, then an intervention located below the dashed line will indicate a larger cost saving than the minimum indicated as acceptable by the dashed line. Paradoxically, then, a less effective intervention need not be a Wasted Buy — as long as it is also sufficiently cheaper than the comparator it will replace. It may even be a Best Buy!
Various techniques have been used to define thresholds. The three most popular methods35 are:
- deriving the threshold from previous decisions or other jurisdictions,
- the willingness to pay of the payer (‘demand-side method’), or
- value of displaced services (‘supply-side method’).
The latter two have gained popularity and are the most cited approaches. However, each has limitations. The demand-side approach requires the society’s or the government’s willingness to pay (WTP) for healthcare to determine the threshold that would guide expenditures from the healthcare budget accordingly. In most cases, society’s willingness to pay will be set explicitly or implicitly by the government. The chosen threshold will inevitably be controversial, so the methods used to determine it should be well-founded, clear and transparent. Where experts are consulted, they should be of appropriate distinction and independence. Calculating an aggregate social willingness to pay by asking citizens is also fraught with difficulties and can be controversial. The WHO previously adopted the approach of the first bullet in the list above. It generated a global threshold ratio taking the form that interventions costing less than three times the average per capita income per disability-adjusted life-years (DALY) averted were considered to be cost-effective and those exceeding this level were considered to be cost-ineffective.36 Subsequently, there was an updated suggestion that the threshold could be between one to three Gross Domestic Product (GDP) per capita.37 This approach in both cases implicitly assumed that there is fixed relationship between GDP and the appropriate magnitude of expenditure on healthcare, despite this being a policy decision that can legitimately vary depending on local priorities. Context and additional considerations38 are matters that should be considered prior to the implementation of any threshold. A global threshold for all countries is an average (which may be generally too high or too low) but will rarely exactly fit the conditions in any particular country and may lead countries into committing themselves to merely Contestable Buys or, worse, to Wasted Buys.39
The threshold, though potentially useful, is not itself a decision rule. It is only a guide. There may be circumstances under which a country may rationally choose to admit interventions that have ICERs above the threshold or reject some that lie below it. For analyses that try to take account of factors other than cost-effectiveness in deciding whether an intervention is a Best Buy, one may turn to Health Technology Assessment (HTA).
Cost-saving and cost-effectiveness are not synonyms. Depending on the context, it is possible, especially in a highly resource-constrained setting, that a less expensive and slightly less effective strategy is preferable, and vice-versa; interventions that are expensive may be cost-effective if they result in significant health outcomes and the cost-effectiveness threshold is sufficiently high.
These, then, are the basic ideas around which this book is built. What initially seems clear, and even obvious, turns out to be complex, controversial and may require the tools of Health Technology Appraisal (HTA) rather than those of CEA alone.
1.5 The Story of This Book
The Prince Mahidol Award Conference (PMAC) was first convened in 2007 and has continued annually since. This global health forum honors the memory of Prince Mahidol of Songkla, who dedicated his life’s work to advancing public health and medical practice in Thailand and is respectfully regarded as the Father of Modern Medicine and Public Health of Thailand. Further information about PMAC is available via this link: https://pmaconference.mahidol.ac.th/site.
At a preparatory meeting for PMAC 2019, the slow progress towards global NCD targets was a major topic for discussion, particularly how the inadequate implementation of effective NCD prevention interventions contributes to this failure. Dr. Yot Teerawattananon, the founding leader of the Health Intervention and Technology Assessment Program (HITAP), emphasized that inefficiency in healthcare hinders progress. Working in collaboration with the International Decision Support Initiative (iDSI) (https://www.idsihealth.org/), which is a network of priority-setting organizations, HITAP has found that low-value health interventions are a significant contributor to wasteful spending in health.
With the financial support from PMAC, the Thai Health Promotion Foundation and iDSI, and in collaboration with several other global partners, HITAP developed a concept note for a practical guide to assist program managers in identifying good solutions (Best Buys) and avoid poor choices (Wasted Buys) for the prevention of NCDs. The concept note was accepted by the PMAC Scientific Committee in Tokyo in May 2018 and the initiative ‘Non-Communicable Disease Prevention: Best Buys, Wasted Buys and Contestable Buys’ was born.
1.6 The Project and Its Output
The project brought together experts from various disciplines in health economics, health policy, political economy, public health practice and NCDs. HITAP, which served as the project’s secretariat, invited various organizations and individuals in its wider network to join the authorship team. In total, we have 20 authors from 14 organizations in 8 countries. Authors were assigned a chapter from the concept note according to their expertise; some chapters were co-authored by members of several organizations. The output was always conceived as something much more than a book. Our findings were to be disseminated through knowledge translation materials such as videos, blogs, animations and interactive seminars. The project aimed to create an evidence package to support health program managers when thinking about NCD prevention. The evidence package as finalized includes the printed book, the online book, online appendices (which include further details on the project, such as additional descriptions on methods), interview clips with policy-makers on the topic of NCD prevention, and a website.40 More details can be found on the project website: https://www.buyitbestncd.health.
1.7 The Project Journey
An initial in-person meeting was held in August 2018 for 12 members of the project team. This meeting enabled the project team members to meet one another and enabled the authors to present and receive comments on the outlines they had developed. Additionally, discussions prompted modifications to the form and structure of the book.
It was recognized that the work needed to be relevant to the target audience of NCD managers, that it should be written in comprehensible language and that it should draw whenever possible on managers’ perceptions and experience. HITAP subsequently put out a call for LMIC-focused case studies on experiences of Best Buys, Wasted Buys or Contestable Buys in the prevention of NCDs. The call was circulated through various channels including: PMAC, iDSI, HTAsiaLink and WHO. In total, 58 case studies were received from thirty countries (https://www.buyitbestncd.health/about). Out of the fifty-eight cases submitted, forty-seven case studies that were deemed relevant were analyzed (see Chapter 4 on Best Buys).
A second, two-day, in-person meeting was convened in November 2019 with chapter leads, the editorial team, project organizers and observers. The preliminary drafts of the findings for each chapter were circulated with authors beforehand and systematically discussed. The concept note originally had the title Best Buys, Wasted Buys and ‘Do-It-Yourselves’ (DIYs) in NCD Prevention. The DIY term was dropped after much discussion, mainly because of its apparent endorsement of an individualistic approach to NCDs, and was replaced by ‘Contestable Buys’ to cover the many cases where Best and Wasted Buys could not be identified unambiguously.
Our initial ideas and some draft chapters were presented in January 2019 at PMAC 2019 (http://pmac2019.com/site) through two side-meetings and one main parallel session. The first side-meeting took the form of a closed meeting where eighteen external reviewers commented on the work to date. A second side-meeting was convened privately for authors to discuss how best to move forward following the feedback received in the previous side-meeting. This discussion resulted in some changes to the proposed content structure of the book and a commitment as far as possible to draw on real-world cases to illustrate points of principle and their practical application. A main parallel session at PMAC 2019 was open to the entire conference. Lead authors presented their chapters for five minutes followed by interactive questions and answers. This session was the best attended parallel session at PMAC 2019 and provided the basis for the final shape and content of the book.
After further draft revisions and editing, chapters and book were sent to ten experts for external review: each of the eight main chapters were assigned a reviewer, and two reviewers were entrusted with evaluating the book as a whole. After further revisions, the chapters were shared with the editorial team for final edits.
1.8 Target Audience
This book is written mainly with individuals who coordinate and/or have decision-making authority over NCD programs in mind. While their official job titles vary, we used the term ‘NCD program managers’ to encompass chronic disease or NCD managers, policy officers, project managers, scheme managers, implementers and evaluators operating in (non-)governmental organizations. Some of the common characteristics of the job roles and the managers’ working environments are as follows. They:
- work in (non-)governmental ‘NCD units’ or ‘sub units’ dedicated to one or more of the main diseases (cardiovascular disease, diabetes, chronic lung disease, cancers and mental health) under the NCD umbrella, or to NCD risk factors;
- implement NCD health plans to the community;
- operate at the national, provincial, district or local level; and/or
- work on the integration of NCDs into existing service delivery platforms.
The target audience of this book thus consists of individuals who work in spheres of implementation. The work is, however, also intended to aid NCD champions, policy advocates and educators who spearhead the movement for increased visibility of NCDs and a reduction in the occurrence of these diseases.
1 Our World In Data, What Do People Die From?, 2018, https://ourworldindata.org/what-does-the-world-die-from
2 World Health Organization, Non-communicable Diseases, 2018, https://www.who.int/news-room/fact-sheets/detail/noncommunicable-diseases
3 Institute for Health Metrics and Evaluation, Global Burden of Disease (GBD), 2019, http://www.healthdata.org/gbd
4 World Health Organization Newsroom, Obesity and Overweight: Key Facts, 2018, https://www.who.int/en/news-room/fact-sheets/detail/obesity-and-overweight
5 International Diabetes Federation, IDF Diabetes Atlas — 8th Edition, 2017, https://diabetesatlas.org/resources/2017-atlas.html
6 World Health Organization, 10 Facts on Non-communicable Diseases, 2019, https://www.who.int/features/factfiles/noncommunicable_diseases/facts/en/index4.html
7 World Health Organization, Tools for Implementing WHO PEN (Package of Essential Non-communicable Disease Interventions), 2019, https://www.who.int/ncds/management/pen_tools/en/
8 World Health Organization, The SHAKE Technical Package for Salt Reduction, 2016, https://apps.who.int/iris/bitstream/handle/10665/250135/9789241511346-eng.pdf?sequence=1
9 World Health Organization, Hearts: Technical Package for Cardiovascular Disease Management in Primary Health Care., 2016, https://apps.who.int/iris/bitstream/handle/10665/252661/9789241511377-eng.pdf?sequence=1
10 David E. Bloom et al., From Burden to ‘Best Buys’: Reducing the Economic Impact of Non-Communicable Diseases in Low-and Middle-Income Countries (Geneva, 2011), http://apps.who.int/medicinedocs/documents/s18804en/s18804en.pdf; David E. Bloom et al., The Global Economic Burden of Non-communicable Diseases, World Economic Forum: World Economic Forum and the Harvard School of Public Health (Geneva, 2011).
11 World Health Organization, World Health Assembly Resolution WHA67.23: Health Intervention and Technology Assessment in Support of Universal Health Coverage (World Health Organization, 2014), http://apps.who.int/medicinedocs/en/m/abstract/Js21463en/
12 United Nations General Assembly, United Nations General Assembly Resolution A/67/L.36: Global Health and Foreign Policy (United Nations, 2012), https://documents-dds-ny.un.org/doc/UNDOC/LTD/N12/630/51/PDF/N1263051.pdf?OpenElement
13 World Health Organization, ‘Non-communicable Diseases: Key Facts 2018’, 2019, http://www.who.int/news-room/fact-sheets/detail/non-communicable-diseases
14 Mauricio L. Barreto et al., ‘Infectious Diseases Epidemiology’, Journal of Epidemiology and Community Health, 60 (2006), 192–95, http://dx.doi.org/10.1136/jech.2003.011593
15 Institute for Health Metrics and Evaluation, Global Health Data Exchange, 2016, http://ghdx.healthdata.org/
16 Ibid.
17 UN Interagency Task Force on NCDs, Working Together for Health and Development: Prevention and Control of Non-Communicable Diseases, 2017, https://www.who.int/ncds/un-task-force/working-together-adaptation.pdf?ua=1
18 Ibid.
19 World Health Organization, 10 Facts on Non-communicable Diseases.
20 Ibid.
21 Catherine P. Benziger et al., ‘The Global Burden of Disease Study and the Preventable Burden of NCD’, Global Heart, 11.4 (2016), 393–97, https://doi.org/10.1016/j.gheart.2016.10.024
22 World Health Organization, ‘10 Facts on Non-communicable Diseases’, https://www.who.int/features/factfiles/non-communicable_diseases/facts/en/index4.html
23 World Health Organization, ‘Non-communicable Diseases: Key Facts 2018’, 2019, http://www.who.int/news-room/fact-sheets/detail/non-communicable-diseases
24 Bloom et al., The Global Economic Burden of Non-communicable Diseases, World Economic Forum: World Economic Forum and the Harvard School of Public Health
25 Dean T. Jamison et al., ‘Universal Health Coverage and Intersectoral Action for Health: Key Messages from Disease Control Priorities’, The Lancet, 11.4 (2018), 1108–20, https://doi.org/10.1016/S0140-6736(17)32906-9
26 World Health Organization, 10 Factors on Mental Health, 2019, https://www.who.int/features/factfiles/mental_health/mental_health_facts/en/index1.html
27 Ibid.
29 Bloom et al., From Burden to ‘Best Buys’: Reducing the Economic Impact of Non-Communicable Diseases in Low-and Middle-Income Countries.
30 The DALY is one of several frequently met measures of the effectiveness of health care interventions. It stands for ‘Disability-Adjusted Life-Year’ where the Life-Year is a year of life gained and an adjustment is then made for the quality of life in terms of presence or absence of disabilities. A measure of health gain is therefore a DALY averted.
31 Michael F Drummond et al., Methods for the Economic Evaluation of Health Care Programmes (Oxford: Oxford University Press, 2015); Andrew Briggs, Mark Sculpher and Karl Claxton, Decision Modelling for Health Economic Evaluation (Oxford: Oxford University Press, 2006).
32 Hilary F. Ryder et al., ‘Decision Analysis and Cost-Effectiveness Analysis’, Seminars in Spine Surgery, 21.4 (2009), 216–22, https://doi.org/10.1053/j.semss.2009.08.003
33 Institute of Medicine (U.S.), Committee on Quality of Health Care in America: Crossing the Quality Chasm: A New Health System for the 21st Century (Washington, DC: National Academy Press, 2001).
34 Jaqueline Zinn and Ann Barry Flood, ‘Commentary: Slack Resources in Health Care Organizations-Fat to Be Trimmed or Muscle to Be Exercised?’, Health Services Research, 44.3 (2009), 812–20, https://doi.org/10.1111/j.1475-6773.2009.00970.x
35 Anthony J. Culyer, ‘Cost-Effectiveness Thresholds in Health Care: A Bookshelf Guide to Their Meaning and Use’, Health Economics, Policy and Law, 11.4 (2016), 415–32, https://doi.org/10.1017/s1744133116000049
36 Tessa-Tan-Torres Edejer et al., ‘Making Choices in Health: WHO Guide to Cost-Effectiveness Analysis’, (Geneva: World Health Organization, 2003), https://www.who.int/choice/publications/p_2003_generalised_cea.pdf
37 World Health Organization, World Health Organization, Cost-Effectiveness Thresholds, 2012, http://www.who.int/choice/costs/CER_thresholds/en/index.html
39 Melanie Y. Bertram et al., ‘Cost-Effectiveness Thresholds: Pros and Cons’, Bulletin of the World Health Organization, 94.12 (2016), 925–30, https://doi.org/10.2471/blt.15.164418
40 The printed, digital and online editions of this book, together with the online appendices, can be found on the Open Book Publishers website, https://doi.org/10.11647/obp.0195

