3. Framework for Implementing Best Buys and Avoiding Wasted Buys
© Chapter’s authors, CC BY 4.0 https://doi.org/10.11647/OBP.0195.03
Best Buys and Wasted Buys are two sides of the same coin. If every healthcare system invested only in Best Buys, then Wasted Buys are automatically avoided. Therefore, if we understand the features of Best Buys, it is straightforward to understand the etiology of Wasted Buys. Best Buy policies are normally based on good intentions, rigorous evidence and efficient management and coordination; by contrast, Wasted Buy policies tend to be formulated with a weak rationale or self-interested motivation, absent or poor-quality evidence, inadequate management and weak coordination. Having a framework of step-by-step practical considerations to implementing Best Buys and avoiding Wasted Buys is consequently to have something of value. With this in mind, we propose the SEED Tool (Systematic thinking for Evidence-based and Efficient Decision-making) as shown in Figure 3.1.
The SEED Tool can be understood broadly in two parts: the inner circle and outer boxes. The inner circle is a set of fundamental questions that NCD policy managers and/or other decision-makers ought to ask themselves. NCD policy managers can increase the likelihood of implementing Best Buys and avoiding Wasted Buys if they systematically take account of each of these considerations. Each is numbered in a normative logical order. Interventions should ideally be assessed sequentially in the following order: sound theoretical basis (1), good quality evidence (2), transferability to the implementation setting (3), reasonable cost (4) and sufficient political investment (5). In practice, however, NCD policy managers may order them differently, depending on their local and political contexts (e.g., starting from five, continuing on to three and then two, etc.). Provided that there are affirmative answers to each consideration, different orderings can still result in a Best Buy. To support this, the outer semi-circle has recommendations on how to incorporate and/or improve evidence support for each of the major considerations. It is important to note that this tool requires political commitment to using evidence for decision-making, which is separate from the political commitment to the intervention under scrutiny (see Consideration 5).
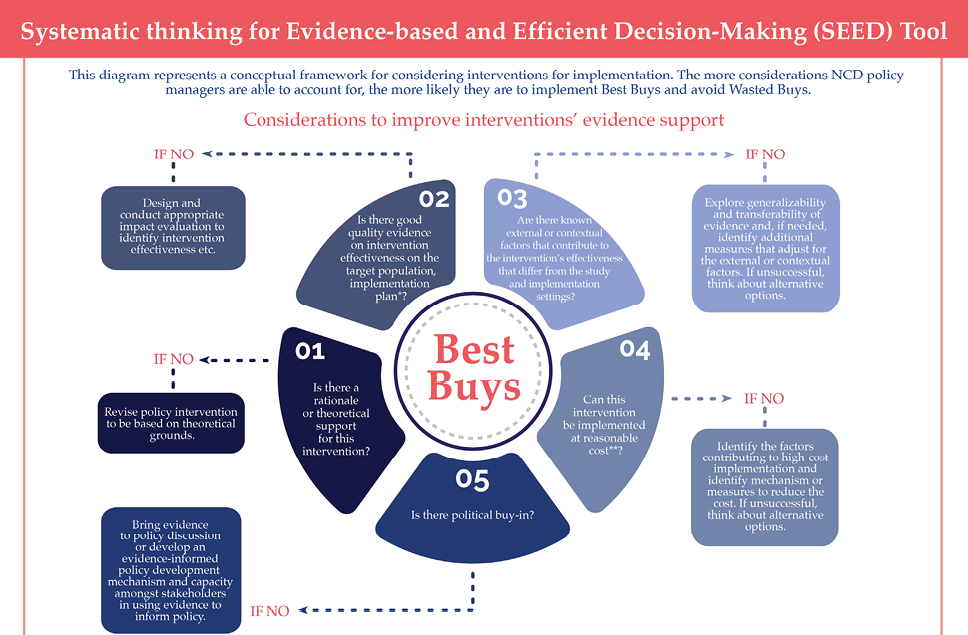
*Implementation = dosage, frequency, duration, coverage, etc.
**In comparison to the cost of implementing a similar program in other settings or compared to the cost parameters used in economic evaluation studies that led to a policy decision to adopt this intervention.
Fig. 3.1 Systematic thinking for Evidence-based and Efficient Decision-making (SEED) tool.
3.1 Consideration One
The first step questions the rationale or the theoretical background for the implementation of the intervention. Unlike curative interventions, where the effect can be observed early, NCD prevention interventions, as with most health-promotion and disease-prevention programs, have indirect effects on disease burdens. They aim to reduce health risks and therefore need a longer timeline to have any measurable impact on disease prevention. If programs do not use tested theories, they may not produce the desired improvements in health.1 The strongest preventative programs have a clear conceptual basis that is built on good evidence. They guide the actual process of planning, implementation and evaluation. Understanding the purpose, history, constructs and context of the situation helps in selecting the most appropriate theory to guide the program. Preventive interventions also generally require commitment from individuals. For example, a mass media campaign to reduce obesity through healthy eating will be effective only if the target population understands and is responsive to the message. Governments can only promote the message but are unable to police healthy eating in the target population. As such, these policies require cultural understanding and should ideally be based on repeated proven experience in the field. This may involve a qualitative rather than a quantitative judgement but should nonetheless be one for which there is persuasive evidence.
3.2 Consideration Two
The second question underlines the need to have good-quality evidence on the effectiveness of any intervention. It is highly desirable that the evidence on intervention efficacy/effectiveness2 should have been tested on the same (or at least very similar) population groups with the same dosage, frequency and other clinical and implementation characteristics — this homogeneity can reduce the risk of bias. There are many excellent appraisal tools for determining the quality of evidence. They are highlighted in an online resource called Enhancing the QUAlity and Transparency of Healthcare Research (EQUATOR) Network.3 This online resource recommends different quality appraisal tools for different type of research. These include: the Consolidated Standards of Reporting Trials (CONSORT) for randomized control trials; the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA); the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE); and the Consolidated Health Economic Evaluation Standards (CHEERS).
Alternatively, the quality of evidence on intervention effectiveness could be evaluated based on the hierarchy of evidence, which ranks different types of studies according to their ‘academic rigor’ (see Fig. 3.2 below and Chapter 7). In this pyramid, the evidence is strongest (lowest potential bias) for systematic reviews and meta-analyses of randomized control trials, followed by randomized control trials, cohort studies, case control studies and case series/reports (and some pyramids also include expert opinion below these other study designs). This hierarchy of evidence exists in various forms in the literature even though most of them have the same general format, with the validity and strength of the evidence based on the risk of bias (also called internal validity).4 While it is helpful to use the hierarchy of evidence, it has limitations in application, especially in LMICs where there is often a lack of quality data or resources to conduct more rigorous study designs.
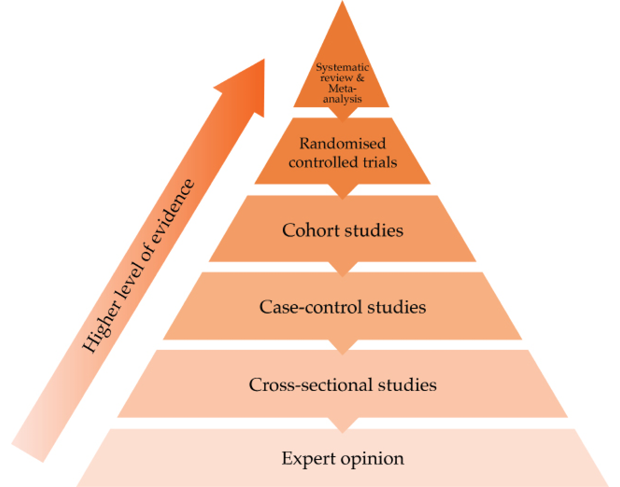
Fig. 3.2 Hierarchy of evidence. Source: Modified from New Evidence Pyramid.5
3.3 Consideration Three
The third question explores whether the studies’ results can be applied to the population of interest and whether the intervention can be transferred to other settings (also called the external validity of the studies). This consideration requires examination of the external or contextual factors that may alter the effect of the intervention from the studies’ settings to the implementation setting. This point is important since many countries (especially LMICs with limited resources for research) use evidence from other countries. An intervention with strong evidence from high-income countries might have less of an effect in more resource-constrained countries due to different population characteristics or a lack of supportive factors (e.g., infrastructure or social norms). Even transferring the study results of an intervention within a country with vastly different regional contexts, such as applying the results of studies set in urban areas to sparsely populated remote areas, can change the intervention effect drastically. The local context, including environmental factors, should therefore always be considered for any studies used for policy-making. NCD managers and policymakers ought to scrutinize the evidence with professional care and ensure that the evidence is reasonably transferable to their context. If this is not the case, then investing in additional measures to address the potential changes in effect, such as training sessions, incentive structures, communications campaigns and awareness raising, should be considered.
3.4 Consideration Four
The fourth question addresses issues related to the cost of the intervention and its budget impact, i.e., cost-effectiveness, affordability and other cost outcomes. When considering a policy, especially preventive interventions where the health harvest is reaped in the future, NCD managers and decision-makers are confronted with higher early healthcare spending from the date of implementation onwards, whereas beneficial health outcomes will come later. Potential Best Buy interventions could be therefore be excluded from the NCD program. In this case, NCD managers should also consider how best to achieve the intervention within the budgetary constraints of the government or health provider; and, specifically to explore whether there are modifiable factors contributing to the high cost of the intervention, such as whether additional capital investment and human resource training will be needed and how they could affect the overall cost or the affordability. Governments, with the benefit of information provided from costing, cost-effectiveness, feasibility and budget impact studies can identify such factors, evaluate the long-term costs and benefits of the intervention and act to reduce the costs, thereby making them affordable and increasing the likelihood of a Best Buy.6
3.5 Consideration Five
The last question asks whether there is political and professional support for the intervention in question. This consideration has different requirements compared to the previous questions, given that it is dependent on factors such as stakeholder consensus and buy-in, social and cultural influences and the governmental structure of the country. This issue is important because a Best Buy might be forgone if there is no political or professional support for it. ‘Policy-informed evidence’ might be deployed in response to high-level political pressures and influences instead of genuine evidence.7 Managing this is tricky, but failure results in the implementation of suboptimal options, especially if this consideration is the first to be addressed in the SEED Tool (one reason for our recommendation to follow the logical order). For example, one of the case studies in this book discusses Thailand’s implementation of a diabetes mellitus and hypertension screening program for the entire population, which was a good political investment even though there was a lack of evidence to support the policy fully.8 An economic evaluation conducted later showed that targeted screening for high-risk groups was more cost-effective and led to a change in policy with the potential for reallocation of the budget to other NCD programs and a further improvement in health outcomes. This case was successful because of a commitment from all sectors. However, it is much better to ensure that policies are based on evidence from the outset and, where this is not established practice, to build a new culture in which it is expected. This implies making sure that professional and training institutions instill in students a clear understanding of evidence-informed decision-making processes and why they are important, and that the training of civil servants and other government officials and advisers likewise includes modules on evidence and decision-making.
3.6 The SEED Tool in Practice
NCD prevention interventions are often complex and multi-faceted, requiring collective effort and time from both public and private players to implement. Consequently, they always come with a high opportunity cost for their introduction or maintenance within healthcare systems. The SEED Tool can be considered a framework or conceptualization that captures all necessary considerations to enhance the probability of implementing Best Buys and avoiding Wasted Buys. Each consideration in the tool has sub-considerations, which are discussed in other sections of this book — as such, the SEED Tool is the backbone of the book and the following chapters on Best Buys and Wasted Buys will illustrate the usefulness of applying it. This SEED Tool is also the starting point for in-depth discussion on technical and practical issues surrounding decision-making processes for health investment, such as the subjects of generalizability and transferability that will be described in Chapter 6 (see the Consideration 3 discussion above) and political buy-in, which is discussed in Chapter 2 as part of its illustration of the political economy of NCD prevention. Governance and process are covered in Chapter 9 (see the Consideration 5 discussion above).
The SEED Tool summarizes not only all the types of evidence — such as those produced in health technology assessments, health systems research, policy studies, etc. — it also incorporates contextual issues such as local intervention costs and political buy-in among key decision makers. Further, given the intricacies of NCD prevention interventions, there are many stakeholders within and outside the health sector with their own perspectives and areas of concern. Having a common framework in the SEED Tool that allows these relevant stakeholders to deliberate and/or prioritize all competing policy options can be crucial for the success of NCD prevention, which requires commitment and ownership at all levels of policy implementation.
This book benefits from using case studies to examine how NCD programs have been implemented in the past; this was an input in developing the SEED Tool. It is designed to be used for considering both new and existing interventions, whether it be for vertical programs or as part of broader public health systems. Specifically, the tool can be helpful in evaluating: 1) the impact of an existing program that will continue to be implemented, and exploring any changes necessary to improve the program; 2) a new program in consideration for implementation; 3) the effect of a program that was completed, to determine lessons learned; and, 4) an ongoing program for continuation. As such, it can be used to evaluate the impact of current or past programs retrospectively as well as to determine whether proposed interventions should be implemented in the future. The authors hope to use and also to test this framework, with the aim of avoiding Wasted Buys and increasing the likelihood of investing in Best Buys.
The tool has the potential to be applied not only for NCDs but also for other public health programs, or even as a system-wide mechanism for priority-setting (for example, as part of the inclusion of health technology or services in the benefits package or the essential medicines list). This tool can also be helpful when used together with priority-setting institutions and appropriate policy processes. This is because the authors believe that together evidence and process can be impactful, generating a loop of better evidence for better processes and vice versa, which eventually leads to better decisions with a greater impact on health.9
1 Carl I. Fertman and Diane D. Allensworth, Health Promotion Programs — From Theory to Practice, 1st edn (San Francisco: Jossey-Bass, 2010), http://soh.iums.ac.ir/uploads/4.pdf
2 Efficacy = intervention performance under ideal and controlled circumstances; effectiveness = intervention performance under ‘real-world’ conditions.
3 Enhancing the QUAlity and Transparency Of Health Research (EQUATOR) Network, The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) Statement: Guidelines for Reporting Observational Studies, 2019, http://www.equator-network.org/reporting-guidelines/strobe/
4 Health Intervention and Technology Assessment Program (HITAP), Guide to Health Economic Analysis and Research (GEAR) Online Resource: Guidelines Comparison, 2019, http://www.gear4health.com/gear/health-economic-evaluation-guidelines
5 M. Hassan Murad et al., ‘New Evidence Pyramid’, Evidence Based Medicine, 21.4 (2016), 125–27, https://doi.org/10.1136/ebmed-2016-110401; Health Intervention and Technology Assessment Program (HITAP).
6 Adun Mohara et al., ‘Using Health Technology Assessment for Informing Coverage Decisions in Thailand’, Journal of Comparative Effectiveness Research, 1.2 (2012), 137–46, https://doi.org/10.2217/cer.12.10
7 Sarocha Chootipongchaivat et al., Factors Conducive to the Development of Health Technology Assessment in Asia: Impacts and Policy Options (Manila: World Health Organization, 2015), https://apps.who.int/iris/bitstream/handle/10665/208261/9789290617341_eng.pdf?sequence=1&isAllowed=y
9 Rob Lloyd et al., International Decision Support Initiative (IDSI) Theory of Change Review Report’, F1000Research, 7.1659 (2018).

