5. Wasted Buys
© Chapter’s authors, CC BY 4.0 https://doi.org/10.11647/OBP.0195.05
5.1 Introduction
In 2011, approximately 6.9 trillion USD were spent globally on health, of which 20–40% were thought by the WHO to be wasted.1 This evidence is corroborated by the Organization for Economic Co-operation and Development (OECD), which found that potentially one-fifth of total health spending in developed countries is wasted.2 This observation is an example of inefficiency, and waste on this scale is far more serious in LMICs, where the overall burden of disease is so much higher and relatively small expenditures can have enormous impact (if spent wisely). The usual methods of controlling rising health expenditures have been either through structural reorganization or cost-cutting measures. The former is time-consuming and carries risks of missing the intended mark, an approach famously lampooned by Maynard in the UK as ‘redisorganization’,3 while the latter is a blunt instrument and may impinge indiscriminately on both cost-effective and cost-ineffective parts of the system. Often the missing piece of this conundrum is figuring out how to eliminate waste and/or low-value health care. Efficiency gains from measures to improve health outcomes can be dispersed across sectors, but also have the potential to allow reallocation from poor value, low-impact interventions to high-value, high-impact ones: a rare win-win for healthcare. Low-value resource allocation exists for a multitude of reasons: lack of evidence needed to create better health outcomes or to identify cheaper but equally effective procedures; poor management and weak coordination; social and political factors that may be of little general benefit to the community; the knowledge deficits and biases of the policy-makers and program managers; and governance-related waste such as fraud and corruption.4
This problem of low-value care is increasingly recognized in clinical medicine.5 Many countries are now promoting the use of generic medicines,6 seeking to prevent unnecessary interventions, avoiding adverse events and improving the targeting of tests and interventions to those most likely to benefit. However, much less is known about inefficient spending on the prevention and control of non-communicable diseases (NCDs) at the programmatic level. This chapter aims to fill this gap.
Our objective is to show that tackling inefficient spending or ‘Wasted Buys’ is a value-enhancing agenda which acts as a catalyzer in achieving the ultimate goals of a healthcare system. We provide an operational, pragmatic definition of Wasted Buys which will help program managers and policy-makers to identify inefficient spending and initiate a constructive dialogue; explain the common characteristics of inefficient spending incurred in the prevention of NCDs with current examples; and show how inefficient spending can be avoided by substituting better care at the same cost, more efficient care (more benefit compared to incremental cost), or cheaper alternatives with the same or even better health outcomes.
5.1.1 What Are ‘Wasted Buys’?
The scalability of any intervention is subject to available evidence, which is often lacking, or is of variable quality, or is not context specific. What constitutes waste is often revealed in an implementation setting that is different from the study setting that generated the existing evidence, so that what might be seen as wasted in one context might not be wasted in another. So how should a program manager identify a Wasted Buy?
The OECD defines ‘waste’ in a developed country context as: (i) services and processes that are either harmful or do not deliver benefits; and (ii) costs that could be avoided by substituting cheaper alternatives with identical or better benefits.7 Developed countries have well-established priority-setting mechanisms and data capture, which can be synthesized into relevant evidence to guide health policy. Developing countries pose a range of challenges in conducting a cost-effectiveness analysis, such as interpreting the poor-quality or non-contextual data used to estimate costs and effects, the choice of the comparator and whether subgroups of the target population are analyzed. There are therefore many uncertainties about how best to proceed. A comprehensive, pragmatic definition that fits the LMIC context is therefore required.
Recalling the analysis of Chapter 1, we treat Wasted Buys as interventions that fall in the shaded area in Figure 5.1, while interventions falling in Section 2 of Quadrant B and the whole of Quadrant D are not Wasted Buys.
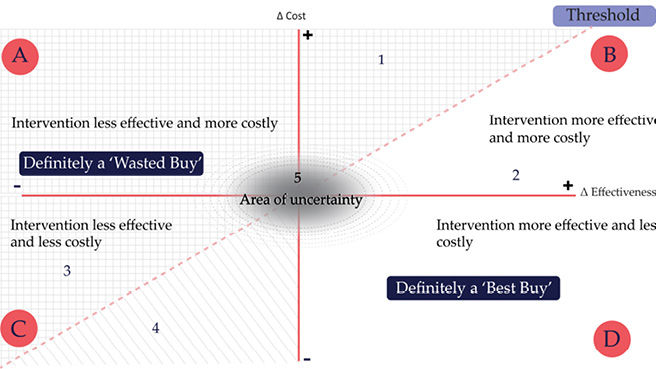
Fig. 5.1 Wasted Buys on a cost-effectiveness plane.
Wasted Buys include interventions that deliver no health benefits (Quadrant A); interventions that yield a higher cost per unit of health outcome gained than the cost-effectiveness threshold in that setting (Section 1 of Quadrant B); and interventions that have low efficacy or no significant positive impact on health outcomes albeit at a meagre cost (Section 3 in Quadrant C). Interventions falling in Section 4 in Quadrant C may need to be deliberated. For instance, interventions with a negative impact may be Contestable or even Best Buys if the cost reduction is sufficiently large to enable more health benefits to be gained elsewhere. Lastly, interventions that have a small cost or benefit impact, or about which there is substantial uncertainty, which fall in the ‘area of uncertainty’ should be carefully scrutinized before implementation (Section 5).
5.1.2 The ‘Area of Uncertainty’
The area of uncertainty (Section 5) has a fuzzy boundary. It has no sharp edges. The area of uncertainty includes interventions that have substantially uncertain benefits or cost-effectiveness. There are three reasons for this. The first is a lack of knowledge and information about the benefits and/or costs of an intervention, as when an intervention is still in the experimental phase or implemented with insufficient understanding of the context. The second is uncertainty around estimations of effect, cost and cost-effectiveness that may come from parameter uncertainty, model uncertainty and uncertainties concerning the assumptions used — for example, in modelling future streams of benefit beyond experimental periods, or in the use of a constant rate of disease incidence over time. Uncertainty afflicts both clinical and economic studies. Finally, generalizability issues occur with proposals to implement an intervention in a new setting with conditions that vary from the study setting.
It is plainly important to note whether the radius of the circle is large or small or, indeed, whether it is a circle. This might remain unknown until further research has been conducted. The importance of understanding these different aspects of uncertainty may also vary across interventions, depending on several factors, such as the infeasibility of some interventions in resource-limited settings. While the cost-effectiveness plane is useful in understanding the types of uncertainty that affect cost, benefit and cost-effectiveness, it does not account for the uncertainties that are unrelated to ex-ante evaluations (conducted prior to the implementation), such as those implicit in the implementation of the intervention itself.
5.2 Exploring Wasted Buys in Low- and Middle-Income Countries (LMICs)
While Best Buys are recognized and widely acknowledged, the existence of Wasted Buys and even Contestable Buys has only just started to gain traction in the health community. The concept of Wasted Buys is broad and examples abound in many countries. To better understand the nature of Wasted Buys, we reviewed the literature to identify studies that illustrated ineffective and cost-ineffective interventions. The review focused on economic evaluations of preventive interventions in non-communicable diseases. We searched the Cochrane Collaboration Database, the Global Health Cost-Effectiveness Analysis (GH CEA) Registry from the Tufts Medical Center and the Disease Control Priorities project.
A. Cochrane Collaboration Database
Effectiveness is a necessary (but not sufficient) starting point to ensure the benefits of an intervention for the health system or to identify a Best Buy. If an ineffective intervention has been implemented, it counts as a low value or a ‘Wasted Buy’. The Cochrane Collaboration database8 is a trustworthy resource and has curated content on the effectiveness of a variety of interventions. We reviewed interventions focusing on negative or inconclusive results. Cochrane reviews related to mass-media campaigns for NCD preventions were selected and are discussed in detail in the next section.
B. The Global Health Cost-Effectiveness Analysis (GH CEA) Registry
We reviewed articles from the GH CEA Registry9 to establish the usefulness of the database and to understand the ‘cost-per-DALY averted’ approach to identifying Wasted Buy interventions. The review covered research conducted in LMICs; research on four specific NCDs: cancer, cardiovascular diseases (CVD), chronic respiratory diseases and diabetes; and intervention(s) for NCD prevention. Interventions were classified as Wasted Buys if the ICER was greater than three times the gross domestic product (GDP) per capita (which is referred to as a proxy for decision-making in LMICs that lack local research on thresholds) or if the ICER was negative, meaning that the intervention is costlier and less effective than the comparator(s). Nine studies were identified, of which one, a study on the cost-effectiveness of medical primary prevention strategies to reduce absolute risk of cardiovascular disease in Tanzania, was selected for review in detail.
C. Disease Control Priorities (DCP)
The three editions of the DCP that have been published focus on cost-effective options according to current research: they highlight potential Best Buys, or interventions that yield the most benefits in terms of health outcomes compared to cost. We reviewed the DCP’s second edition and selected sections of the third to assess the project’s ability to shed light on Wasted Buys as well as Contestable Buys and Best Buys. The following chapters of DCP II were selected: Health Service Interventions for Cancer Control in Developing Countries; Diabetes: The Pandemic and Potential Solutions; Cardiovascular Disease; and Respiratory Diseases in Adults. From DCP III, Volume 3 (Cancer) and Volume 5 (Cardiovascular, Respiratory and Related Disorders) were selected. The DCP authors conducted systematic reviews of high-burden diseases and economic evaluations, including diabetes in developing countries. They explored the interventions that were mentioned as being of lower priority due to cost-ineffectiveness, less clinical benefit, infeasibility and other relevant considerations. They are non-prescriptive and were published without the use of any specific threshold or willingness to pay for an intervention. In addition, many of the studies used different methods and had no standard outcome measures. Since performance of the interventions in the implementation setting is a major consideration in identifying Best or Wasted Buys, interventions from the DCP project require further study or research for their transferability across settings.10
To analyze context-specific factors that might lead to Wasted Buys and that capture the perspective of program managers, we placed a call for case studies (as described in Chapter 1). This was circulated through a variety of networks. Fifty-eight case studies from thirty countries were received. Case studies that were deemed relevant to the NCDs theme were then analyzed (see Online Appendix 4B). A considerable portion of the cases submitted as Best Buys were not based on any evidence other than international guidelines or other countries’ precedents. This is reflected in the case studies on diabetes screening in Indonesia and Thailand and drug testing among civil servants in Bhutan.
Case Study 5.2.1 Leveling up: Mass-media campaigns for prevention of NCDs
Mass-media campaigns can change risk behavior by providing information with messages of warning, empowerment, or support, or offering incentives intended to correct erroneous normative beliefs, clarify social and legal norms, or set positive role models or social norms.11 Several behavioral theories explain the possible relationships through which mass-media interventions can influence health-related behavior by improving knowledge, attitudes and self-efficacy that contribute to a person’s motivation and competence to take appropriate actions.12 Given their potential for population reach, many governments often use mass media to deliver health messages with the intention of improving health literacy and mitigating risky health behavior.
The WHO recommends several mass-media campaigns as Best Buys in NCD prevention.13 These include:
- mass-media campaigns that educate the public about the harms of smoking/tobacco use and second-hand smoke;
- mass-media campaigns to promote healthy diets (including social marketing to reduce the intake of total fat, saturated fats, sugars and salt) and the intake of fruits and vegetables;
- reduced salt intake through a mass-media campaign that aims to change behavior; or
- a mass-media campaign combined with other community-based education, motivational and environmental programs aimed at supporting behavioral change in relation to physical activity levels.
But mass-media interventions might be Contestable Buys. These campaigns are often implemented at relatively high cost, especially when they are administered though newspapers or other printed materials, radio, television, billboards or social media. Our review of three Cochrane publications14 reveals that the available evidence is inadequate to conclude that mass-media campaigns alone can meaningfully change health behavior and/or reduce the burden of NCDs in the target population. Most studies related to mass-media campaigns that are focused on knowledge, attitude, awareness and short-term change in other outcomes (such as service utilizations) lack clear evidence about improvements in health outcomes (such as a reduction in the incidence or prevalence of NCDs).15 There is therefore a need for stringent evaluation of such mass-media campaigns, using studies with a before-and-after design that control for all factors affecting the campaign. They should include qualitative methods to demonstrate impact and unpack the most important elements of the campaigns.16 Mass-media campaigns may have become an established intervention by now, so it could be difficult for NCD managers to accept their failure in terms of evidenced direct health impact. Campaigns may also, however, have value to NCD managers because they generate social and political coverage and may open avenues to engage public support for more effective NCD policies.
This case shows that while mass campaigns are not clear Wasted Buys, targeted mass-media campaigns on their own are inadequate to moderate the growth of NCDs. It is better for these campaigns to be implemented after careful research that supports their use rather than relying on well-meaning but essentially blind faith. This case study lies in Quadrant A (Fig. 5.1) in the area of uncertainty.
Case Study 5.2.2 Overseas and over here: Cost-effectiveness of medical primary prevention strategies to reduce the risk of cardiovascular disease (CVD) in Tanzania
Following the publication of the WHO’s CVD preventive guidelines,17 a research team led by Tanzania’s Ministry of Health and Social Welfare conducted a study on the cost-effectiveness of medical preventive therapies for reducing the absolute risk of CVD.18 Although global evidence reflecting the benefits of preventive medicine in cardiology exists, variation in countries’ circumstances, including demographic, epidemiological, socio-economic and policy contexts, limits the transferability of findings. The Ministry therefore collaborated with academics to produce a local cost-effectiveness study using local data, age-specific background mortality rates and the provider cost of CVD treatment.
The study found that Losartan and Simvastatin, as a combination drug for all risk levels, was successful in averting DALYs. However, Tanzania’s willingness to pay (at that time 610 USD or 1 GDP per capita per DALY averted) was insufficient to warrant proceeding. A recommendation followed that medical treatment should not be provided for low-risk patients without diabetes. This combination drug seemed to be a Wasted Buy. In this case, the threshold was a major determinant in the decision-making process and was explicitly used to identify Wasted Buys.
Tanzania’s study result lies in Section 1 of Quadrant B (Fig. 5.1) because primary prevention intervention is effective but the costs exceed the threshold. This is an example of an intervention that is effective but not cost-effective. If policy-makers were to increase the level of health investment, this would imply higher thresholds and the multi-drug combination may then prove to be good value for money (however, doing this would also increase the likely cost-effectiveness of other, possibly even more efficient, interventions).
Case Study 5.2.3 Streamlining health policy for health gains: Diabetes screening in Thailand and Indonesia
A large element of the NCD burden in Southeast Asia is attributed to diabetes. An estimated 96 million people have diabetes, 90% of whom have the preventable type 2 diabetes.19 Almost half this burden goes undetected, especially among disadvantaged minorities. However, timely diagnosis eases diabetes management and ensures access to appropriate care. Several countries have implemented population-based diabetic screening programs. One such program is the WHO Package of Essential Non-communicable Disease Interventions (WHO PEN). The tools in this package enable early detection and management of the major NCDs. Although screening is widely considered to be an effective strategy, program managers and policy-makers often fail to assess the transferability of the global guidelines.
In Indonesia and Thailand, CVD and diabetes are significant disease burdens. Given the health and financial benefits of screening, these countries’ ministries adapted parts of the PEN guidelines for their primary care public health services. After three years of implementation, an economic evaluation of the PEN package in Indonesia compared to no screening was conducted.20 The findings revealed that implementation of the PEN program was indeed better than no policy, although it could have been improved through a targeted screening policy for high-risk groups aged forty and above, as opposed to the current entry level of fifteen years old. Screening for the fifteen-to-thirty-nine-year-old age category turned out to be a Wasted Buy. The savings from adopting the study recommendations could potentially be invested wisely and efficiently in other areas of priority.
In 2012, Thailand introduced a policy for national diabetes screening annually for people aged fifteen years and above. The policy was solely based on a high-level decision-maker’s judgement following an analysis of the national epidemiological survey, but without considering other important factors such as infrastructure, feasibility, readiness assessment, or affordability. In 2015, an economic evaluation found that a targeted screening program for people aged thirty years and above would be more efficient.21 Here again, screening the fifteen-to-thirty-year-old segment of the population was found to be a Wasted Buy.
The adoption of the new targeted screening policy in Thailand, despite its practicality and financial feasibility, posed a major challenge to policy-makers due to a potential negative public perception of the disinvestment. In Thailand, even though the evaluation was conducted in 2015, implementation took three years and received much resistance from policy-makers. In cases like these, an assessment of the key success factors, as well as the external factors influencing the intervention and their implications in the implementation context, should be considered. Using the SEED Tool detailed in Chapter 3, Considerations Two and Three would help address these points systematically.
Diabetes screening lies in the cost-ineffective region of Section 1 of Quadrant B (Fig. 5.1), because, although screening can be cost-effective, screening the entire population is not.22
Case Study 5.2.4 Back to basics: Drug testing in Bhutan
Lifestyle choices contribute greatly to the burden of NCDs. Smoking, substance and alcohol abuse are notorious culprits. Some countries use workplace drug testing as a common intervention to mitigate the risk of substance abuse. The United States, one of the early adopters, first implemented it in the mid-1980s to ensure drug-free federal workplaces, initially for employees in safety and security jobs. Soon after, new laws allowed public and private companies to drug test their employees.23 Decades later, other countries, including the United Kingdom, Canada and several other European countries, introduced measures allowing drug testing using urine sampling. The reliability of this method is imperfect. Urine drug testing can involve samples that have been diluted; it is unable to differentiate between recreational and habitual use or uses on or without prescription. It is also found that urine samples contain metabolites and little of the parent drug.24
There are often two main objectives in implementing a drug testing program: to reduce substance abuse in the workplace during working hours; or to ensure workplace safety. The effectiveness of workplace drug testing in meeting these objectives is unclear or may have unintended negative outcomes. Two systematic reviews examined the effectiveness of random drug testing aimed at determining whether it reduces injuries and accidents, of which one also examined whether it deterred employee drug use. The studies had methodological limitations and the evidence was insufficient to conclude that drug testing was effective.25 Several studies also found weaknesses in the reviews, such as lack of randomization and test result validation. Drug testing as an intervention should therefore be undertaken with caution.26 In the United States, research shows that employee drug testing often does not reduce employee substance abuse but may have the effect of excluding abusers from the workplace entirely.27 If the goal is to reduce substance abuse by individual employees and ensure that they are on the path to quitting, additional measures are needed to provide guidance and therapy for current drug users, whose cost-effectiveness would also of course require testing. Screening alone appears to have little to no bearing on quitting rates.
These issues do not disappear when LMICs implement similar policies without thoroughly examining the evidence. Bhutan implemented a pre-employment drug-testing scheme for its Royal Civil Service Commission (RCSC).28 The RCSC aimed to eliminate substance abuse in the government as well as to support the general national effort to deter abuse. The policy suffered some of the pitfalls mentioned above: 1) the tests were administered by human resource officers without adequate quality checks of the results; 2) while the twenty-four-hour notification to the employee prior to testing was a rule, the actual implementation was questionable; 3) of the 1,682 new employees in 2017, only two tested positive, so the positive test rate was low, which might be accurate or might be due to prevalent false negative test results; and 4) though the employees were sent to a Drugs Counselling Centre for guidance, there were no further measures. Further, there are no concrete interventions to address substance abuse by current employees.
The SEED Tool recommends that one should first examine the theoretical grounds for implementation as well as the existing evidence to ascertain the policy’s a priori viability in meeting its aims. Given that there are clinical and implementation issues as well as weak evidence for this intervention, the NCD managers could choose to revise the policy or change it entirely. For example, other interventions, such as health promotion detailing the dangers of substance abuse and intensive therapy, could be implemented alongside the testing. This case lies in Quadrant A as a Wasted Buy near or in the area of uncertainty (Fig. 5.1).
5.3 Common Features of Wasted Buys
These case studies reveal common features of Wasted Buys. They often result from misguided motivations and beliefs, as well as from political, institutional, managerial, economic and social pressures and rigidities pervading the decision-making and implementation sphere of NCD management. The following summarizes some of the main features: 1) the fallacy that prevention interventions are always Best Buys; 2) one size seldom fits all in international guidelines; 3) policy-based evidence versus evidence-based policy; 4) selective implementation of interventions; and 5) low CE threshold used for decision-making.
5.3.1 The Fallacy that Prevention Interventions Are Always Best Buys
The case studies show that NCD managers, decision-makers and stakeholders are vulnerable to an inaccurate generalization to the effect that preventive interventions are always both effective and cost-effective and so can significantly reduce the burden of the disease (the ‘prevention is better than cure’ mantra). Such beliefs persist because of a lack of reliable evidence about the true impact of prevention. Many also believe that national scaling-up of a preventive intervention increases the benefits gained. This may not always be the case, as was found in Indonesia and Thailand’s diabetic screening of a young population.
5.3.2 One Size Seldom Fits All in International Guidelines
It is evident from the case studies in Indonesia, Tanzania and Thailand, as well as from many other countries not described here, that there is much uncritical adoption of international recommendations and guidelines in the belief that they are a gold standard. Even when they develop their own guidelines, countries tend to incorporate international recommendations without contextualization. Disease factors and incidence, health-system infrastructure and the cost of intervention often change the calculated cost-effectiveness of interventions. Uncritical acceptance of studies done in other, more developed countries imparts a systematic bias when applying results to LMICs. This is a problem of the transferability of prevention guidelines from one setting to another. International recommendations are rarely tailored to the economic levels of countries, whether low-income, upper/middle-income, or high-income. They are generally based on an analysis of all countries with a natural focus around the mean. In this case, recommendations may be applicable to half of all countries that require them, but not to the rest (see Fig. 5.2) — for example, in the case of evaluating an anti-hypertensive medicine with a price range that varies globally. While this seems like a doom-and-gloom scenario for countries beginning the formulation of their NCD programs, international guidelines can still be a useful starting point for policy consideration and priority-setting — but they do require careful scrutiny of methods and evidence, and may sometimes require detailed analysis of subgroups via a systematic review or, whenever feasible, further locally-focused research.
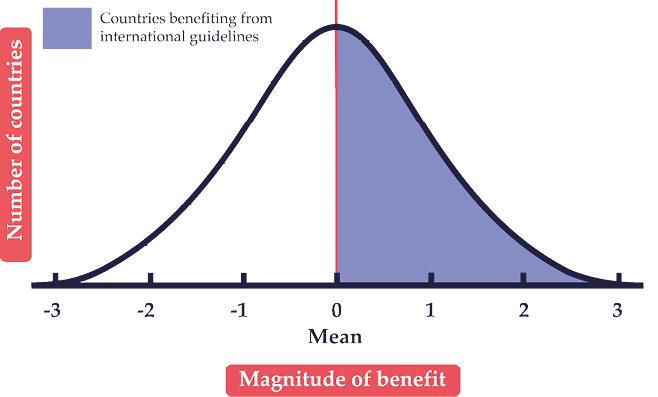
Fig. 5.2 Normal distribution of countries benefitting from international guidelines.
5.3.3 Policy-Based Evidence Versus Evidence-Based Policy
Policies can sometimes be developed without strong evidential support, because they are supported instead by the interests or passions of high-level decision-makers, or by pressures from stakeholder groups. Such policies are likely to result in Wasted Buys. For example, one case study demonstrated that a high-level politician was a zealous supporter of diabetes mellitus screening, for which they then sought evidence to support implementation. This selective use of evidence is a form of exclusion bias. While ‘political engagement and support’ is an extremely important part of the policy-making process and is required to implement the policy, the SEED Tool places it as a final check to prevent ‘policy-based evidence’ and reduce the likelihood of a Wasted Buy.
5.3.4 Selective Implementation of Interventions
NCDs are complex diseases requiring multi-layered interventions. However, some case studies, such as the Bhutan drug-testing program and the mass-media campaign for NCD prevention, make it evident that countries often implement an intervention, policy or technology that is untested or has conflicting or unconvincing evidence of effectiveness. This scenario may be due in part to the first common feature of Wasted Buys, which is a belief in preventive interventions as inevitable Best Buys. A related case is the implementation of interventions that have positive effects but have been shown to require additional interventions to ensure a more substantial impact relative to other interventions, or that are effective but too costly. ‘Too costly’ in this context means that a greater health benefit would have been generated had the money been spent on other interventions, or in other sectors. This is a classic area where an ‘on-paper’ Best Buy results in either a Contestable or Wasted Buy due to incomplete understanding of the cost-effectiveness criterion, pre-judgment and bias, inappropriate inferences about studies that have been done elsewhere and poor or incomplete implementation.
5.3.5 Low CE Threshold Used for Decision-Making
Even a threshold that is low by international standards of cost-effectiveness can cause an intervention to be a Wasted Buy because a threshold that is not set sufficiently low will lead to more recommended additions to the benefits package than the budget can sustain. There are many ways of determining this threshold.29 The right threshold may be hard to discern but it should not be set arbitrarily. An ICER that admits more interventions than are affordable is too high, so the judgment of affordability (i.e., what the budget will support) is very important. It is much more common for thresholds, whether explicit or implicit, to be set too high than too low. One way of judging the right level of the threshold is to model the likely consequence of (a) small rises or falls in it and (b) small rises or falls in the healthcare budget allocation. Such experimentation ought to indicate clearly whether the threshold should be set higher or lower.30 The tendency to set thresholds too high encourages Wasted Buys and may cause true Best Buys to be crowded out by interventions that have a much lower impact on the public’s health.
5.4 Recommendations
Our goal has been to assist NCD managers and other stakeholders in navigating a pathway from Wasted to Best Buys in their own local context. But what ought one to do to correct past commitments to Wasted Buys that are still present in the system? The science of ‘reversing’ such commitments is evolving, but the intellectual guidance provided in this Wasted-Buy chapter still holds. To avoid future Wasted Buys, or to reverse an existing one, requires similar analysis and a similar commitment. There needs to be:
- due deliberation about the additional31 considerations;
- collective acknowledgment of the existence of Wasted Buys — that they may entail sunk costs but nevertheless are diverting resources from higher-value applications;
- an awareness that it is critical to generate good will — political, professional and social — for broader stakeholder support and the process of carrying out reform, involving ongoing stakeholder consultation and participation;
- a high-level commitment to ensure that priority-setting is part of an explicit, formal and well-resourced policy agenda beyond short-term political timelines;
- transparent decision-making frameworks removed from vested interests;
- clear objectives and nomenclature, articulating an ethic of waste reduction and minimizing opportunity costs rather than rationing;
- and finally, substantial new resources for data collection, monitoring, analysis and sharing.32
Further, and to conclude, we recommend the following principles when considering any intervention:
- follow the step-by-step SEED Tool for considering whether to implement an intervention or not. Not all preventive measures, even those recommended in international guidelines, can be assumed to be Best Buys — their health impact (relative to other opportunities) may not be worth the investment, depending on a variety of contextual factors;
- develop agendas and policies in a participatory and systematic way with adequate checks and balances and involvement of all relevant stakeholders, to increase policy scrutiny and reduce the likelihood of ‘policy-based evidence’;
- consider whether the reason why an intervention might be cost-ineffective, and therefore a Wasted Buy, could be related to the cost and outcome components. For example, the intervention cost may be higher in the implementation setting compared to the study setting;
- seek ways of turning an intervention into a Best Buy, such as cutting or minimizing high-cost items without adversely affecting effectiveness. Identify the factors affecting outcomes and whether there are contextual circumstances that limit the impact of the intervention;
- consider whether there is a tenable case for a selective intervention even though, based on evidence, it should be coupled with other interventions as part of a package to address the outcome;
- lastly, if the intervention has a relatively low ICER but remains cost-ineffective according to the average thresholds used in the literature, consider whether the average threshold is even roughly appropriate for your setting.
1 World Health Organization, Global Health Expenditure Atlas (Geneva: WHO Press, 2014), https://www.who.int/health-accounts/atlas2014.pdf
2 OECD, Tackling Wasteful Spending on Health, 2017, https://www.oecd.org/health/tackling-wasteful-spending-on-health-9789264266414-en.htm
3 Alan Maynard, ‘What about Value for Money?’, BMJ, 342 (2011), https://doi.org/10.1136/bmj.d1319
4 Vikas Saini et al., ‘Addressing Overuse and Underuse around the World’, The Lancet, 390 (2017), 105–7, https://doi.org/10.1016/S0140-6736(16)32573-9
5 Shannon Brownlee et al., ‘Evidence for Overuse of Medical Services around the World’, The Lancet, 390 (2017), 156–68, https://doi.org/10.1016/S0140-6736(16)32585-5
6 OECD, ‘Pharmaceutical Spending Trends and Future Challenges’, in Health at
a Glance 2015 (Paris: OECD Publishing, 2015), https://www.google.com/search?q=Pharmaceutical+Spending+Trends+and+Future+Challenges&oq=Pharmaceutical+Spending+Trends+and+Future+Challenges&aqs=chrome..69i57j0.831j0j4&sourceid=chrome&ie=UTF-8
7 OECD, Tackling Wasteful Spending on Health.
8 ‘Cochrane | Trusted Evidence. Informed Decisions. Better Health’, 2019, https://www.cochrane.org/
9 Center for the Evaluation of Value and Risk in Health (CEVR) Tufts Medical Center, ‘Global Health CEA Registry’, 2019, http://healtheconomics.tuftsmedicalcenter.org/ghcearegistry/
10 K. M. Venkat Narayan et al., ‘Diabetes: The Pandemic and Potential Solutions’, in Disease Control Priorities in Developing Countries, 2nd Edition (Washington, DC: Oxford University Press, New York The International Bank for Reconstruction and Development/The World Bank, 2006).
11 Marica Ferri et al., ‘Media Campaigns for the Prevention of Illicit Drug Use in Young People’, Cochrane Database of Systematic Reviews, 5.6 (2013), CD009287, https://doi.org/10.1002/14651858.CD009287.pub2
12 Jane T. Bertrand et al., ‘Systematic Review of the Effectiveness of Mass Communication Programs to Change HIV/AIDS-Related Behaviors in Developing Countries’, Health Education Research, 21.4 (2006), 567–97, https://doi.org/10.1093/her/cyl036; Jeff Niederdeppe et al., ‘Media Campaigns to Promote Smoking Cessation among Socioeconomically Disadvantaged Populations: What Do We Know, What Do We Need to Learn, and What Should We Do Now?’, Social Science and Medicine, 67 (2008), 1343–53, https://doi.org/10.1016/j.socscimed.2008.06.037
13 David E. Bloom et al., From Burden to ‘Best Buys’: Reducing the Economic Impact of Non-Communicable Diseases in Low-and Middle-Income Countries (Geneva, 2011), http://apps.who.int/medicinedocs/documents/s18804en/s18804en.pdf
14 Malgorzata M. Bala et al., ‘Mass Media Interventions for Smoking Cessation in Adults’, Cochrane Database of Systematic Reviews, 2013, https://doi.org/10.1002/14651858.CD004704.pub3; Malcolm P. Brinn et al., ‘Mass Media Interventions for Preventing Smoking in Young People’, in Cochrane Database of Systematic Reviews, ed. by Kristin V. Carson (Chichester, UK: John Wiley & Sons, Ltd, 2010), https://doi.org/10.1002/14651858.CD001006.pub2; Annhild Mosdøl et al., ‘Targeted Mass Media Interventions Promoting Healthy Behaviours to Reduce Risk of Non-Communicable Diseases in Adult, Ethnic Minorities’, Cochrane Database of Systematic Reviews, 12.2 (2017), 200 https://doi.org/10.1002/14651858.CD011683.pub2
15 Ruth G. Jepson et al., ‘The Effectiveness of Interventions to Change Six Health Behaviours: A Review of Reviews’, BMC Public Health, 10.1 2010, https://doi.org/10.1186/1471-2458-10-538
16 Melanie A. Wakefield, Barbara Loken and Robert C. Hornik, ‘Use of Mass Media Campaigns to Change Health Behaviour’, The Lancet, 376.9748 (2010), 1261–1271, https://doi.org/10.1016/S0140-6736(10)60809-4
17 World Health Organization, Prevention of Cardiovascular Disease: Guidelines for Assessment and Management of Total Cardiovascular Risk, Nonserial Publication (Geneva, Switzerland: World Health Organization, 2011).
18 Frida N. Ngalesoni et al., ‘Cost-Effectiveness of Medical Primary Prevention Strategies to Reduce Absolute Risk of Cardiovascular Disease in Tanzania: A Markov Modelling Study’, BMC Health Services Research, 16.1 (2016), 1–29, https://doi.org/10.1186/s12913-016-1409-3
19 ‘Addressing Asia’s Fast Growing Diabetes Epidemic’, Bulletin of the World Health Organization, 95.8 (2017), 550–51, https://doi.org/10.2471/blt.17.020817
20 Waranya Rattanavipapong et al., ‘One Step Back, Two Steps Forward: An Economic Evaluation of the PEN Program in Indonesia’, Health Systems and Reform, 2.1 (2016), 84–98, https://doi.org/10.1080/23288604.2015.1124168
21 Yot Teerawattananon et al., ‘Development of a Health Screening Package under the Universal Health Coverage: The Role of Health Technology Assessment’, Health Economics (United Kingdom), 25 (2016), 162–78, https://doi.org/10.1002/hec.3301
22 Rattanavipapong et al.; Teerawattananon et al.; Wangchuk Dukpa et al., ‘Is Diabetes and Hypertension Screening Worthwhile in Resource-Limited Settings? An Economic Evaluation Based on a Pilot of a Package of Essential Non-Communicable Disease Interventions in Bhutan’, Health Policy and Planning, 30.8 (2015), 1032–43, https://doi.org/10.1093/heapol/czu106
23 Michael R. Frone, Alcohol and Illicit Drug Use in the Workforce and Workplace, Choice Reviews Online (Washington, DC: American Psychological Association, 2013).
24 Michael R. Levine and W. P. Rennie, ‘Pre-Employment Urine Drug Testing of Hospital Employees: Future Questions and Review of Current Literature’, Occupational and Environmental Medicine, 61.4 (2004), 318–24, https://doi.org/10.1136/oem.2002.006163
25 C. M. Cashman et al., ‘Alcohol and Drug Screening of Occupational Drivers for Preventing Injury’, Cochrane Database of Systematic Reviews, 2.13 (2009), https://doi.org/10.1002/14651858.cd006566.pub2; Timothy Christie, ‘A Discussion of the Ethical Implications of Random Drug Testing in the Workplace’, Healthcare Management Forum, 28.4 (2015), 172–74, https://doi.org/10.1177/0840470415581251; Michael T. French et al., ‘To Test or Not to Test: Do Workplace Drug Testing Programs Discourage Employee Drug Use?’, Social Science Research Academic Press, 2006, 33.1, 45–63, https://doi.org/10.1016/s0049-089x(03)00038-3
26 P. Homo et al., ‘Workplace Drug Testing: An Overview of the Current Situation’, Journal of Toxins, 3.1 (2016), https://doi.org/10.13188/2328-1723.1000013; Isabel Kazanga et al., ‘Prevalence of Drug Abuse among Workers: Strengths and Pitfalls of the Recent Italian Workplace Drug Testing (WDT) Legislation’, Forensic Science International, 215.1 (2012), 46–50, https://doi.org/10.1016/j.forsciint.2011.03.009; Hilde Marie Erøy Lund et al., ‘Results of Workplace Drug Testing in Norway’, Norsk Epidemiologi, 21.1 (2011), 55–59, https://doi.org/10.5324/nje.v21i1.1426; Michael T. French et al.; Shin Yu Lin et al., ‘Urine Specimen Validity Test for Drug Abuse Testing in Workplace and Court Settings’, Journal of Food and Drug Analysis, 26.1 (2018), 380–84, https://doi.org/10.1016/j.jfda.2017.01.001
27 Christie, ‘A Discussion of the Ethical Implications of Random Drug Testing in the Workplace’.
28 RCSC, ‘Notifcation-on-Drug-Test’, 2017, https://www.rcsc.gov.bt/wp-content/uploads/2017/08/Notifcation-on-Drug-Test.pdf; RCSC, ‘Bhutan Civil Service Rules and Regulations’, 2018, https://www.rcsc.gov.bt/wp-content/uploads/2018/05/BCSR2018.pdf
30 Anthony J. Culyer, ‘Cost-Effectiveness Thresholds in Health Care: A Bookshelf Guide to Their Meaning and Use’, Health Economics, Policy and Law, 11.4 (2016), 415–32, https://doi.org/10.1017/s1744133116000049
32 Adam G. Elshaug et al., ‘Levers for Addressing Medical Underuse and Overuse: Achieving High-Value Health Care’, The Lancet, 390.10090 (2017), 191–202, https://doi.org/10.1016/s0140-6736(16)32586-7

